Emergency Hyperbaric Oxygen Therapy – A Service in Need of Resuscitation
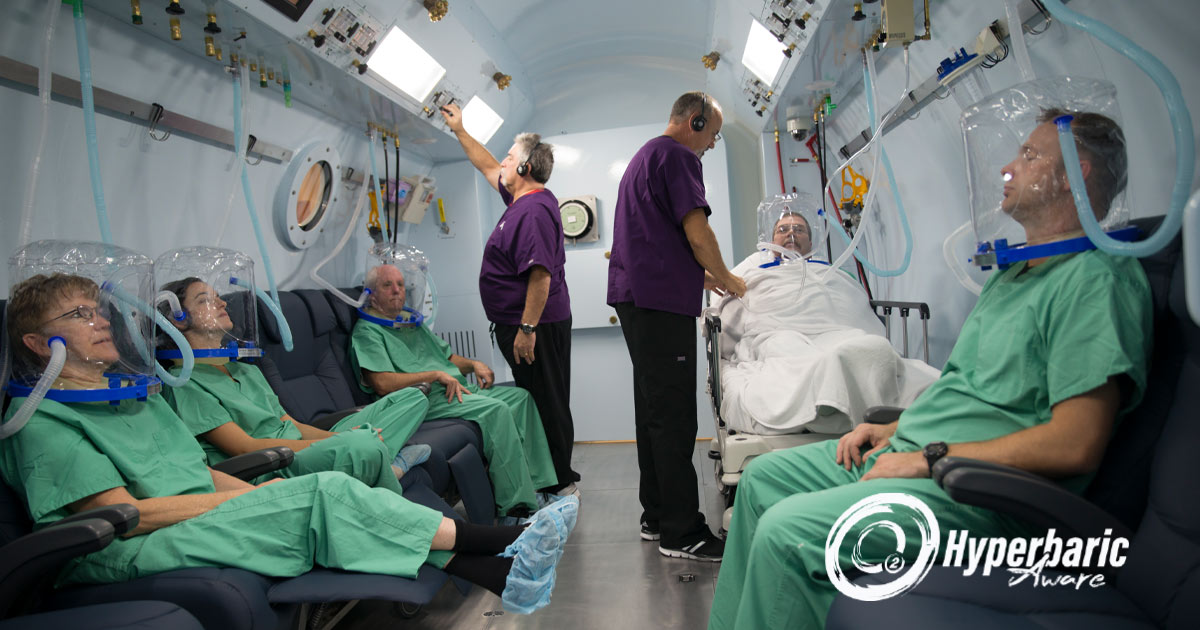
The availability of emergency hyperbaric medicine is a constant concern to its practitioners in the United States. And with good reason.
Each year in the United States approximately 70,000 patients need emergency hyperbaric oxygen (HBO2) treatment, but many facilities cannot take them. Today fewer than 10% of the approximately 1,300 U.S. hyperbaric facilities will accept emergency HBO2 patients. Two decades ago most hyperbaric treatment facilities offered emergency HBO2.
Why the downturn?
The reasons for the loss of emergent hyperbaric medicine include these issues:
- Money: Health care facilities get a better economic return when chambers focus on wound care patients as opposed to emergencies;
- Liability: A greater legal liability is involved with treating high-acuity emergency patients; and
- Lack of training: Emergency operations may require increased training and staffing requirements to manage critically ill patients (especially diving injuries and iatrogenic gas embolism patients).
Shortfalls hurt
Although the rest of medicine in our country is advancing, this current shortage represents a serious decline in the quality of U.S. health care. This shortage of emergent HBO2 availability means that patients with a number of disorders may suffer. Diving-related conditions as well as thromboembolic, iatrogenic (i.e., caused by medical investigation or treatment), traumatic, and infectious conditions can result in death, permanent neurological damage, permanent loss of vision, or loss of an extremity – most of which could have been readily preventable had emergent hyperbaric medical treatment been administered.
A minority of the patients who need this lifesaving HBO2 therapy are within the immediate catchment area of a major hospital with a 24-hour emergency hyperbaric facility. Despite the urgent need for treatment, most hyperbaric chambers will decline to accept emergent patients at present. Patients may eventually receive HBO2 but after a significant delay and a transfer of several hundred miles. Many never receive indicated HBO2, often resulting in poorer patient outcomes.
UHMS working to turn this trend around
What can be done about this? In the late summer of 2020 the Undersea and Hyperbaric Medical Society, in partnership with the American College of Surgeons, the American College of Emergency Physicians, the Divers Alert Network, the Academy of Underwater Arts and Sciences, and other organizations sent a letter describing this significant deficiency in U.S. health care to the President, selected cabinet members and elected representatives both in Congress and at the state level to bring this to their attention. The letter included a variety of topics for lawmakers to consider.
- Chambers must be incentivized to offer 24/7 emergent HBO2 therapy;
- More physicians must be trained in hyperbaric fellowship programs approved by the Accreditation Council for Graduate Medical Education;
- Chambers must be protected from crushing legal liability when they accept critical patients; and
- Organizations like the Divers Alert Network, which help connect patients who badly need emergent HBO2 therapy with hyperbaric treatment facilities able to provide this care, must be encouraged and supported.
The following letter is a start, but the medical, diving, and military communities must all continue working together to find solutions for this problem.
Frank K. Butler, MD
Richard E. Moon, MD
(Free access available at: https://www.uhms.org/publications/pressure-new/pressure-pdfs/2020-pressure/third-quarter-pressure-2020.html – Pages 12-16)
The letter: A good start
22 August 2020
To: (Each addressee received a separate letter)
President of the United States of America
Chair and Members of Appropriate House and Senate Committees
Secretary of Defense
Secretary of HHS
Administrator of CMS
Secretary of DHS
Secretary of Interior
Secretary of Transportation
Governor of Florida
Governor of Alabama
Governor of California
Governor of Hawaii
American Hospital Association
We are writing to express our concern about the decreasing availability of emergent access to hyperbaric oxygen (HBO2) therapy in many areas of the United States, including a growing number of major population centers.
A number of disorders – including diving-related, thromboembolic, iatrogenic (caused by medical investigation or treatment), traumatic, and infectious conditions – may cause loss of life, permanent neurological damage, permanent loss of vision, or loss of an extremity if not treated emergently with hyperbaric oxygen.
Delays in obtaining HBO2 treatment reduce or eliminate the possibility of obtaining a good outcome for these patients. Each year in the United States, there are approximately 400 serious cases of decompression illness in divers; almost 1,000 reported cases of arterial gas embolism (gas bubbles in the arteries, or AGE) occurring as a result of medical or surgical procedures; 50,000 cases of carbon monoxide poisoning; 6,200 cases of acute blindness due to occlusion of the central retinal artery; and 13,000 cases of life-threatening soft tissue infections. Failure to provide prompt access to HBO2 therapy for these conditions is a clear departure from the evidence-based, best-practice standard of care.
There are approximately three million recreational scuba divers in the U.S. In the unlikely event that they suffer a diving-related injury, they trust that the U.S. medical system will provide state-of-the-art care for their injuries, but the steadily decreasing number of hyperbaric treatment facilities in the U.S. willing to treat them emergently for decompression sickness or arterial gas embolism often places them at much greater risk than they realize.
In May of 2020, a retired Marine Corps aviator made a dive to 70 feet for 20 minutes off the coast of Pensacola, Florida. He was battling a large speared fish near the end of his dive. After surfacing, he experienced serious neurological symptoms that were indicative of a diving-related injury, but none of the five hyperbaric treatment facilities in Pensacola currently provide the emergency HBO2 therapy that he badly needed. Knowing that no hyperbaric treatment facilities in the city or in the rest of Northwest Florida would treat the injured diver, his dive buddy, a retired Navy flight surgeon, arranged for him to be transported to the hyperbaric facility at Springhill Medical Center, in Mobile, Alabama, the closest treatment facility that offers emergency HBO2 therapy, where he was treated successfully. This facility continues to offer emergent HBO2 despite the fact that it is not financially advantageous to do so. (The owners of the Springhill facility, the Wallace family, do this as a public service for the Gulf Coast diving community.) As described in the attached white paper, treatment delays such as occurred during this patient’s care, are one of the most significant risk factors for a negative outcome when treating patients with decompression sickness or arterial gas embolism.
This reduced capability to provide emergency treatment for diving accidents also impacts local fire and police forces, many of which have diving rescue teams; federal law enforcement agencies; fish and wildlife services, park service and other state and federal agencies with dive teams; as well as military divers conducting training operations in areas away from the location of their unit chamber; all of these divers also would not be able to receive optimal care if there is no emergent HBO2 treatment available in proximity to their operations.
There are approximately 1,300 hyperbaric treatment facilities (each of which has one or more hyperbaric chambers) that currently provide HBO2 therapy in the United States. As recently as two decades ago, the large majority of hyperbaric treatment facilities were available to provide emergent HBO2 treatments on a 24/7 basis, but today, fewer than 10% of these facilities offer emergency HBO2 treatment, and some of those facilities do so only intermittently. Electively scheduled patients being treated for wound healing deficiencies dominate the remainder of chamber usage, with some additional chambers used in support of civilian and military diving operations.
As a business enterprise the scheduled wound care model is much more profitable than emergent HBO2 therapy. In the past, hospitals and other hyperbaric treatment facilities underwrote the additional costs associated with providing 24/7 access to emergent HBO2 as a public service for patients who require it. Now, because of funding and staffing considerations, as well as concern for legal liability, most hyperbaric treatment facilities have ceased to provide 24/7 access to emergent HBO2 therapy.
There is an urgent need to correct this decreasing availability in the U.S. health care system and make emergent HBO2 available to those patients who require it.
This will require the identification and implementation of strategies to incentivize hyperbaric treatment facilities to offer emergent HBO2 therapy. Options for accomplishing this include:
1) direct federal or state grants to hyperbaric treatment facilities that offer emergent HBO2;
2) indemnification from legal liability for hyperbaric treatment facilities and medical providers who provide emergent HBO2 to divers and other patients who require it;
3) recognition of the public service performed by the hyperbaric treatment facilities that offer HBO2 on an emergent basis when indicated;
4) favorable consideration with respect to Medicare, Medicaid, and private insurance reimbursements to hyperbaric treatment facilities and medical providers that offer HBO2 on an emergent basis when indicated, including carve-outs to inpatient DRG (diagnosis-related group) payments;
5) incentives for military hyperbaric facilities to provide emergent HBO2 to civilian patients through emphasis on the training benefit to military providers that this accomplishes; third-party reimbursement for emergency HBO2 therapy provided to civilian patients by military hyperbaric facilities; and indemnification of the military facility from lawsuits resulting from this public service activity.
In addition, there should be federal support for non-profit organizations willing to operate around the clock assisting any patient who needs emergent HBO2 therapy by identifying the nearest hyperbaric treatment facility that is capable of providing this treatment and helping to arrange transportation to it. Since chamber availability may vary based on ongoing HBO2 treatments, staffing issues, and chamber maintenance operations, the ability to quickly determine which hyperbaric treatment facility is the most appropriate for a particular emergency patient in a specific geographic area is critical to optimal care. It should likewise be a national health care priority to ensure that there is adequate funding for fellowship education in Hyperbaric Medicine so that appropriately trained physicians will be reliably available to oversee the HBO2 therapy provided by these hyperbaric treatment facilities.
Please see the accompanying white paper for additional detail on this important aspect of emergency health care. We would like to have representatives from our organizations meet with you regarding this worsening deficiency in the U.S. health care system.
(Free access available at: https://www.uhms.org/publications/pressure-new/pressure-pdfs/2020-pressure/third-quarter-pressure-2020.html – Pages 12-16)
Sincerely,
American Academy of Underwater Sciences
Academy of Underwater Arts and Sciences
American Board of Wound Healing
American College of Emergency Physicians
American College of Hyperbaric Medicine
American College of Surgeons
Association of Dive Program Administrators
Divers Alert Network
National Association of Underwater Instructors
National Board of Diving & Hyperbaric Medical Technology
Professional Association of Diving Instructors
Texas Medical Association
Undersea and Hyperbaric Medical Society
University of California San Diego Division of Hyperbaric Medicine and Wound Care
Categories
Contributing Specialists

